Gum disease is one of the most common threats to long-term oral health, and it often progresses quietly until it reaches an advanced stage. At Lake Harris Dental, our goal is to help patients recognize risks early, preserve natural teeth, and protect the tissues that hold the smile in place. This page explains how periodontal disease develops, what to watch for, and how modern treatment approaches stop progression and restore health whenever possible.
Understanding periodontal disease starts with knowing what the tissues around your teeth are and how bacteria, inflammation, and everyday habits interact. The information below is written to give you clear, practical insight without unnecessary jargon so you can take confident next steps if you or a loved one needs care.
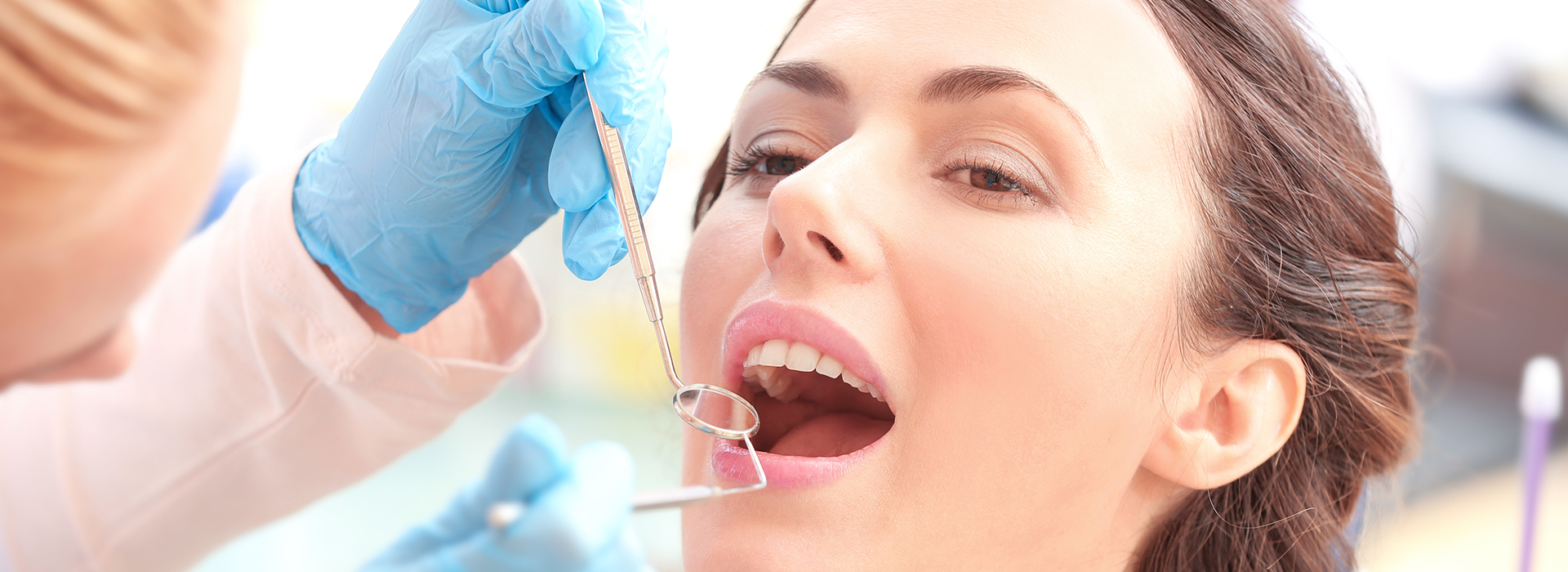
Gum disease starts when bacteria in dental plaque accumulate along the gumline and around tooth roots. Early on, this triggers inflammation of the gum tissue as the body responds to microbial irritants. If plaque and tartar are removed regularly, inflammation often resolves; if not, the reaction can intensify and move deeper into the tissues that support each tooth.
As inflammation becomes persistent, it damages the connective tissue and the tiny fibers that anchor teeth to bone. Over time pockets form between the tooth and gum where bacteria can thrive, making it harder to remove the source of infection with routine brushing. This progression—from mild inflammation to destructive infection—is why early diagnosis and consistent care are so important.
Periodontal disease is not identical for every person. Genetics, medical conditions, smoking, certain medications, and oral hygiene habits all influence how quickly the disease advances. A tailored treatment plan addresses both the infection and the contributing factors so that healing can occur and long-term stability can be achieved.
Common signs that warrant a periodontal evaluation include:
Gums that appear red, puffy, or otherwise inflamed
Bleeding during brushing, flossing, or spontaneously
Noticeable gum recession exposing more of the tooth’s root
Increased sensitivity to hot, cold, or sweet stimuli
Persistent bad breath or an unpleasant taste in the mouth
Teeth that feel mobile or shifting position
New gaps forming between teeth or changes in bite alignment
Partial dentures that no longer fit properly
Fluid or discharge near the gumline
Discomfort when biting or chewing food

Oral health and overall health are connected. Chronic gum inflammation affects the body’s inflammatory balance and has been associated with conditions such as diabetes, cardiovascular disease, and respiratory illness. While the exact relationships are complex, maintaining periodontal health reduces sources of chronic inflammation and supports general well-being.
Preserving the tissues that surround teeth also preserves function—chewing, speech, and facial support depend on healthy gums and bone. When periodontal disease progresses, the cumulative loss of supporting tissue can lead to tooth loss and the need for more extensive restorative care.
Prevention, early detection, and consistent maintenance are the most reliable ways to limit the broader impact of periodontal disease. Partnering with your dental team to manage risk factors and follow an individualized maintenance schedule is a practical approach to protecting both oral and systemic health.
Gingivitis is the earliest, reversible form of gum disease. It shows up primarily as red, tender, or bleeding gums but does not yet involve permanent loss of bone or connective tissue. Because symptoms can be mild, many people assume bleeding is normal and delay addressing the cause.
Treatment for gingivitis focuses on eliminating plaque and tartar and restoring healthy oral hygiene habits. A professional cleaning combined with improved brushing and flossing techniques can remove the inflammation and return gum tissue to a healthy state. Regular re-evaluation confirms that the condition has been controlled.
Early intervention not only prevents escalation into more destructive stages but also keeps care less invasive. When gingivitis is treated promptly, full recovery of the gum tissue is the expected outcome in most cases, underscoring the importance of routine dental visits.

When gingivitis is not controlled, it can progress to periodontitis, a stage where the infection damages the connective tissue and the jawbone that stabilize teeth. Clinically, this stage is identified by increased pocket depth around teeth, detectable bone loss on x-rays, and possible gum recession.
As pockets deepen, bacteria become more difficult to remove with home care alone, and the resulting environment perpetuates inflammation and tissue breakdown. Left untreated, periodontitis can lead to progressive tooth mobility and ultimately tooth loss.
Management of periodontitis aims to halt the destructive process, reduce pocket depth, and preserve as much natural tissue and bone as possible. Successful outcomes combine mechanical removal of the bacterial challenge, targeted use of adjunctive therapies when indicated, and a personalized maintenance program to prevent recurrence.
Periodontal care begins with a comprehensive assessment that measures pocket depths, evaluates gum recession, reviews radiographs, and identifies contributing factors such as systemic health or habits. This diagnostic step allows the dental team to design a treatment plan that is specific to the patient’s needs and realistic goals.
Conservative treatments are the first line of defense when possible; when deeper disease is present, more involved therapies may be required. Throughout care, the emphasis is on controlling the bacterial source, resolving inflammation, and restoring an environment where oral tissues can heal and stay healthy.
We work closely with patients to set expectations, explain each procedure in plain language, and establish a long-term schedule for professional maintenance—this combination leads to better stability and improved chances of preserving natural teeth.
Non-surgical periodontal therapy is the foundation for treating early to moderate disease. The most common procedure—scaling and root planing—removes plaque and hardened deposits from beneath the gumline and smooths root surfaces so the gums can reattach more effectively.
Adjunctive measures, when appropriate, include localized antimicrobial applications or systemic medications to help reduce the bacterial load. These options are selected based on clinical findings and the patient’s overall health, aiming to minimize invasiveness while achieving meaningful improvement.
After non-surgical therapy, careful re-evaluation determines whether healing has occurred or if further treatment is needed. Many patients experience significant improvement and can maintain periodontal health with regular maintenance visits and strong home care.
When disease has advanced to the point where pockets are too deep for effective nonsurgical cleaning, surgical options are considered. Procedures such as flap surgery allow clinicians to access deep areas for thorough debridement, to reduce pocket depth, and to reshape affected tissue for easier maintenance.
Regenerative techniques—like bone grafts and tissue-guided regeneration—are available to rebuild lost support in select cases. These procedures aim to restore the bony architecture and connective tissues so that teeth have improved stability and function.
Modern surgical care also includes less invasive technologies such as laser-assisted therapy in appropriate situations. The decision to proceed surgically is guided by clinical evidence, diagnostic imaging, and a frank discussion about goals and expected outcomes.
When periodontal disease is identified and managed effectively, the outlook for maintaining teeth and oral function is far better than many people expect. If you have questions about any of the topics covered here or would like to schedule an evaluation, please contact us for more information. Our team at Lake Harris Dental is ready to help you protect and preserve your smile.

Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Lake Harris Dental, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
Periodontal disease is an infection of the tissues that surround and support the teeth, driven by bacteria that collect in plaque and hardened deposits. It begins as inflammation of the gums and can progress deeper into the connective tissues and bone if not controlled. The course and severity vary by individual, with genetics, medical conditions, and habits influencing progression.
The process typically starts when plaque accumulates along the gumline and stimulates a local immune response. Persistent plaque and tartar allow bacteria to flourish in pockets that form between tooth and gum, making infection harder to remove with routine home care. Early diagnosis and targeted treatment interrupt this cycle and improve the chances of preserving natural teeth.
Common early signs include gums that are red, swollen, or tender and bleeding during brushing or flossing. Patients may also notice persistent bad breath, an unpleasant taste, or increased sensitivity to hot and cold. Because symptoms can be subtle, many people do not recognize these warnings as signs of disease.
Gum recession, new gaps between teeth, or teeth that feel loose are indications the condition may be advancing. Any of these changes should prompt a periodontal evaluation so clinicians can measure pocket depths and determine whether non-surgical treatment or further care is needed. Timely attention keeps treatment less invasive and outcomes more predictable.
Diagnosis begins with a clinical exam that measures pocket depths around each tooth and inspects gum tissue for inflammation and recession. Radiographs are used to assess bone support and detect areas of bone loss that are not visible during the exam. The dental team also reviews medical history, medications, and lifestyle factors to identify risks that affect healing and treatment planning.
Additional tests may include charting tooth mobility and checking for bleeding on probing to gauge disease activity. This comprehensive assessment allows clinicians to classify disease severity and design a personalized plan that addresses both the infection and contributing factors. Clear communication about findings helps patients understand goals and expected steps in care.
Non-surgical care is the first line of therapy for early to moderate disease and centers on scaling and root planing, a deep cleaning that removes plaque and hardened deposits from beneath the gumline. Smoothing root surfaces reduces bacterial reservoirs and gives gums a better chance to reattach to tooth roots. Treatment is typically performed under local anesthesia when needed to maximize patient comfort.
When indicated, adjunctive measures such as localized antimicrobial applications or short courses of systemic medication may be recommended to reduce bacterial load. After initial therapy, the clinician re-evaluates healing and pocket depths to determine whether additional treatment is needed. Many patients achieve stability with this approach combined with improved home care and regular maintenance visits.
Surgery is considered when pockets are too deep for effective non-surgical cleaning or when regenerative procedures are needed to restore lost support. Flap surgery provides direct access for thorough debridement, allows reduction of pocket depth, and reshapes tissue for improved maintenance. Surgical intervention can also reposition tissue to reduce sensitivity and improve the fit of prosthetic devices when required.
Regenerative techniques such as bone grafting and guided tissue regeneration aim to rebuild lost bone and connective tissue in selected cases to improve tooth stability. Less invasive options, including laser-assisted therapies, may be appropriate in certain situations to reduce bacterial burden and support healing. The choice of surgical technique is guided by clinical evidence, imaging, and a frank discussion of goals and realistic outcomes.
Systemic conditions such as diabetes can increase the risk and severity of periodontal disease because they alter the body’s inflammatory response and impair healing. Poor glycemic control is associated with greater susceptibility to infections and slower recovery after periodontal treatment. Conversely, controlling blood sugar helps reduce periodontal inflammation and improves treatment outcomes.
Other systemic factors, including certain medications and immune disorders, also influence periodontal risk and the choice of therapies. Coordinated care between a patient’s medical providers and dental team is important when systemic health issues are present. Patients should inform the dental team about their medical history and current medications to ensure safe, effective treatment planning.
The earliest stage of periodontal disease, gingivitis, is reversible with professional cleaning and diligent home care because there is no permanent bone or connective tissue loss. Treating gingivitis promptly typically allows gum tissue to return to a healthy state and prevents progression. Regular professional reevaluation confirms that inflammation has resolved and that oral hygiene is effective.
Once periodontitis has caused measurable bone or connective tissue loss, those structural changes cannot be fully reversed in all cases, although treatment can arrest progression and in some circumstances partially restore lost support. Regenerative procedures may rebuild bone and connective tissue in select patients, improving stability and function. Long-term success depends on controlling the bacterial challenge and maintaining a strict maintenance schedule.
Recovery time varies with the type and extent of treatment but most patients experience mild to moderate discomfort, swelling, and sensitivity that improve over several days to weeks. Clinicians typically recommend simple measures such as gentle brushing in treated areas, short-term use of antiseptic rinses, and avoiding hard or crunchy foods while tissues heal. Any prescribed medications should be taken as directed to control pain and reduce the risk of infection.
Follow-up visits allow the dental team to monitor healing, remove sutures when present, and reassess pocket depths to confirm improvement. Patients should report persistent or worsening pain, excessive bleeding, or unusual discharge so the team can address complications promptly. Following the recommended home-care routine and attending maintenance appointments are key to sustaining long-term health.
Consistent daily oral hygiene is the most important preventive measure and includes thorough brushing twice a day and cleaning between teeth once daily with floss or interdental brushes. Tobacco cessation significantly lowers periodontal risk because smoking impairs blood flow and immune response in gum tissue. Regular professional cleanings and periodontal evaluations help catch early changes before they progress.
Managing systemic health conditions such as diabetes, maintaining a balanced diet, and taking medications as prescribed also support periodontal health. For patients with increased risk, the dental team may recommend more frequent maintenance visits, targeted antimicrobial therapies, or specialized home-care tools. Active partnership with the dental team and adherence to recommended routines reduce the likelihood of recurrence.
Our approach begins with a thorough assessment that identifies disease severity, contributing factors, and patient goals so we can design a clear, personalized plan of care. We combine evidence-based non-surgical therapies with selective use of advanced surgical and regenerative techniques when indicated, and we explain procedures in plain language to set realistic expectations. Emphasis on patient education and comfortable, minimally invasive methods helps patients participate actively in their own care.
Long-term maintenance is tailored to each patient’s needs and typically includes scheduled periodontal cleanings, regular pocket charting, and risk factor management to prevent recurrence. By working together with patients and their medical providers when necessary, we aim to preserve natural teeth and support overall health. If you have concerns about your gum health or would like to schedule an evaluation, our team at Lake Harris Dental is available to help.

Looking to book your next dental visit or need more information about our services?
Getting in touch with Lake Harris Dental is simple and stress-free. Our welcoming team is happy to help you schedule an appointment, explain treatment options, and answer any questions you may have. Whether you choose to call, email, or use our easy online contact form, we’re ready to assist you. Take the next step toward a healthier, more confident smile by contacting us today and experience dental care tailored just for you.